Providing Optimal Ways for Processing Insurance Claims
Processing health care insurance claims is an uphill task for healthcare providers. And during critical times, like that of a pandemic, the number of transactions can overwhelm your billing department. Improper management of insurance claims processing can lead to costly errors and even compliance violations. Delegating claims processing healthcare to a medical claims’ management company is the best available option for providers to save on money and time expended in managing the process and ensuring accuracy and compliance.
MedBillingExperts effectively integrates technology, experienced personnel, and flexibility to provide end-to-end medical insurance claims processing services. We understand that for every claim that is not closed on-time, the administrative costs incurred will go up. For that reason, we strive to reduce the open-to-close ratio for our clients. From our team of experienced domain experts to our established processes and from our global delivery centers to our modern claims management system, we ensure every claim is processed correctly for clearance at the very first submission.
We
Help You
Minimize Claims
Processing
Errors.
Here’s
How:
- Organize front office process to verify patient eligibility accurately contact insurer for verifying coverage and policy changes
- Automate billing tasks that are routine and repetitive. Some such tasks include issuing payment reminders, cross verifying medical codes etc.
- Ensure multiple quality checks of files at different stages of the claims process. We also carry out regular audits of the QC process.
- Track denials for at least 3 months to develop a baseline ratio of denials to charges and focus accordingly on claim form corrections
- Be up to date with payer deadlines and process claims before the deadline. Establish a process to understand delays in claims submissions
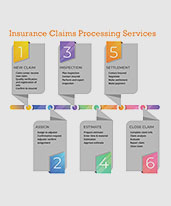
Our medical insurance claims processing steps consist of the following
Review Claim Forms
Receive new claims check for eligibility and errors in coding and billing
Check for Payer Rules
Pre-adjudicate the claim to make it accurate and in keeping with payer guidelines
File Claims
File the processed claim with the insurance company and get claim status number
Review Denials
Receive and review denied claims and resubmit them for review
Follow up
Follow up with payers on resubmitted claims or wrong denials
Our Insurance Claims Processing Support Services Cover Your End-to-End Needs
Our health insurance claim process helps you to make your healthcare claims processing system more streamlined and better managed:
Eligibility Check
Checking patient eligibility is a critical part of our medical claims processing service. We carry it out meticulously to have a clear understanding of primary and secondary coverage details, out-of-network benefits, and patient’s payment obligations. Our streamlined eligibility check service helps our clients to eliminate all types of delays in insurance claims processing.


Billing and Reconciling of Accounts
Our billing and reconciliation services help you to submit accurate claims and receive detailed reconciliation reports of billing data and payments from various payers. These reports provide a detailed break of the payments received, denied charges and outstanding bills. We review the reports and flag inconsistencies with the payer. We do regular follow ups till the issue gets settled.
Open-To-Close Claim Ratio
We assist our clients in reducing claims submission errors and, in the process, improve open-to-close claim ratio. We adopt best-of-the-breed techniques and technologies – fraud control technology, understanding of deep internal codes, automated systems for chosen areas – to ensure all types of errors in claims forms are identified and eliminated.


Robust Quality Control
We guarantee quality healthcare claims processing services by banking on system enhancements to streamline workflow, centralizing information to reduce touchpoints, and leveraging data analytics to take informed decisions. We have created well-defined workflows to ensure accurate and consistent results day-in and day-out.
Review Denial Decisions
At times, a payer may process a claim incorrectly. In such cases we get in touch with the insurance company to figure out why a claim was rejected. If after evaluating the denial reasons we believe it was processed incorrectly at the payer’s end, we write a formal appeal for a review seeking a reconsideration of their decision.

Our Specialties
- Acupuncture
- Allergy / Immunology
- Andrology
- Anesthesiology
- Audiology
- Ambulance Billing
- ASC Billing
- Bariatrics
- Cardiology Billing
- Chiropractic Billing
- Clinical Summary
- Clinical Chemistry
- Clinical Virology
- DME Billing
- EMS Billing
- Dentistry
- Dermatology
- Discharge Summary
- Emergency Room
- Emergency Medicine
- EMR
- EHR
- Endocrinology
- Environmental Medicine
- ENT Neurology
- Epidemiology
- Family Medicine
- Forensic Medicine
- Family Practice Billing
- Gynecology Billing
- Genetics
- Geriatrics
- Hematology
- History and Physical reports
- Hospital Billing
- Internal Medicine Billing
- IME / Peer Reviews
- Infectious Disease
- Internal Medicine
- Medical Documentation
- Medical Records Summary
- Mental Health Billing
- Neonatology
- Nephrology
- Neurology Billing
- Nuclear Medicine
- Occupational Therapy
- Obstetrics
- Occupational Medicine
- Otolaryngology Billing
- Operative reports
- Ophthalmology
- Optometry
- Orthopedics
- Osteopathy
- Otolaryngology
- Pain Management
- Pathology Billing
- Pharmacy Billing
- Pediatric Billing
- Plastic Surgery Medical Billing
- Patient Charts
- Psychiatry/Psychology
- Physician Billing
- Radiology Billing
- Urgent Care Billing
- Pediatric Neurology
- Surgery/Surgery Notes
- Pediatric/Geriatric reports
- Pediatrics
- Physical therapy
- Physiotherapy
- Plastic Surgery
- Podiatry
- Preventive Medicine
- Progress Notes
- Pulmonology
- Radiation Oncology
- Radiology
- Reproductive Medicine
- Rheumatology
- Skilled Nursing Facility
- SOAP notes
- Speech Therapy
- Sports Medicine
- Teleconferences
- Urgent Care
- Urology
- Vascular Medicine
- Gastroenterology/
Gastrointestinal - Rehabilitation Reports/
Medicine
Why we are an Industry Authority in Insurance Claims Processing Services
HIPAA Compliance
As a HIPAA compliant healthcare BPO service provider we follow standard transactions to improve claims management revenue cycle.
Extensive Training
Our team of claim processors are trained continuously to be up to date with the rules and regulations of third-party payers.
High Accuracy
The claim files undergo multi-level quality checks to ensure there is complete accuracy in information filed.
Rigorous Claim Audits
We carry out regular audits of our claims insurance process to identify procedural lapses and plug them to keep the process optimized.
Assured Data Security
Our healthcare insurance claims process is conducted through secure networks fortified by firewalls VPNs, SSLs, and advanced encryption techniques.
Advanced Technology
We deploy advanced claims processing tools and software to eliminate errors and ensure a quick turnaround.
How we Streamline Healthcare Insurance Claims Process
Meticulous Filings
We meticulously file claims after verifying patient eligibility, coverage status, and demographic information
Multiple Reviews
We carry out multiple reviews of the claims forms to ensure that primary and secondary insurance details and coding is accurate
Payer Rules
Our claims processing experts have updated knowledge of each payer requirements and process claims form accordingly.
Read What our Clients have to Say About Us
Roger Scudder Renowned Ambulance Service Provider, Texas
"We were facing huge claims mismanagement which was leading to denials. Soon our revenue loss began to mount to unprecedented levels. MedBillingExperts helped us find out that the main reasons for our denials were charge entry errors and erroneous information. We sought the help of MedBillingExperts and they helped us streamline the process in 2 months’ time. Our losses were completely reversed. I will always say the claims processing staff at the company are amazing! Every question I had, they responded on time. Now thanks to them we have a more stable process in place."
Dr Fritz General Manager, Reputed Cardiology Center, Washington
"Lack of resources and high volume of claims led to missing of deadlines in filing claims. Our inhouse processors had to deal with huge number of claims in a day and were overwhelmed with the workload. To top it, incoming claims continued to pile up.MedbillingExperts provided us with adequate number of staff to deal with our mounting problems. Their robust process ensured there was no erroneous claims submissions and no pile up of backlogs. Soon, we got full control over the claims filing process."
Health Insurance Claims Processing Through Our lens
Infographics
The Importance of Healthcare Insurance Verification and Ways to Streamline It
Insurance verification is a critical part of the insurance claims process. This infographic takes you through all the major steps of insurance verification that can well be the founding stone to smooth claims processing.
View our infographic hereBlog
Know the Features that Make an Insurance Verification Tool Powerful and Reliable
Insurance verification consists of several sequential steps, one of which is verifying patient eligibility. By relying on a patient eligibility verification tool, providers can make this task a lot easier. This blog throws light on the essential features that a verification tool must unmistakably have.
Read more infoCase Studies
Meeting Insurance Eligibility & Benefits Verification Challenge
We assisted Minnesota's largest medical billing and consulting service provider, working with over 100+ accounts (Clients/Doctors) across multiple specialties process, simplify the complex and time-consuming process of verifying patient insurance coverage.
Read case study to know more97%
Clean Claims On First Submission24/7
Support100%
HIPAA Compliance25%
Increase in CollectionsGet a Quick Quote
Our Healthcare Software Expertise


 1-866-344-1936
1-866-344-1936